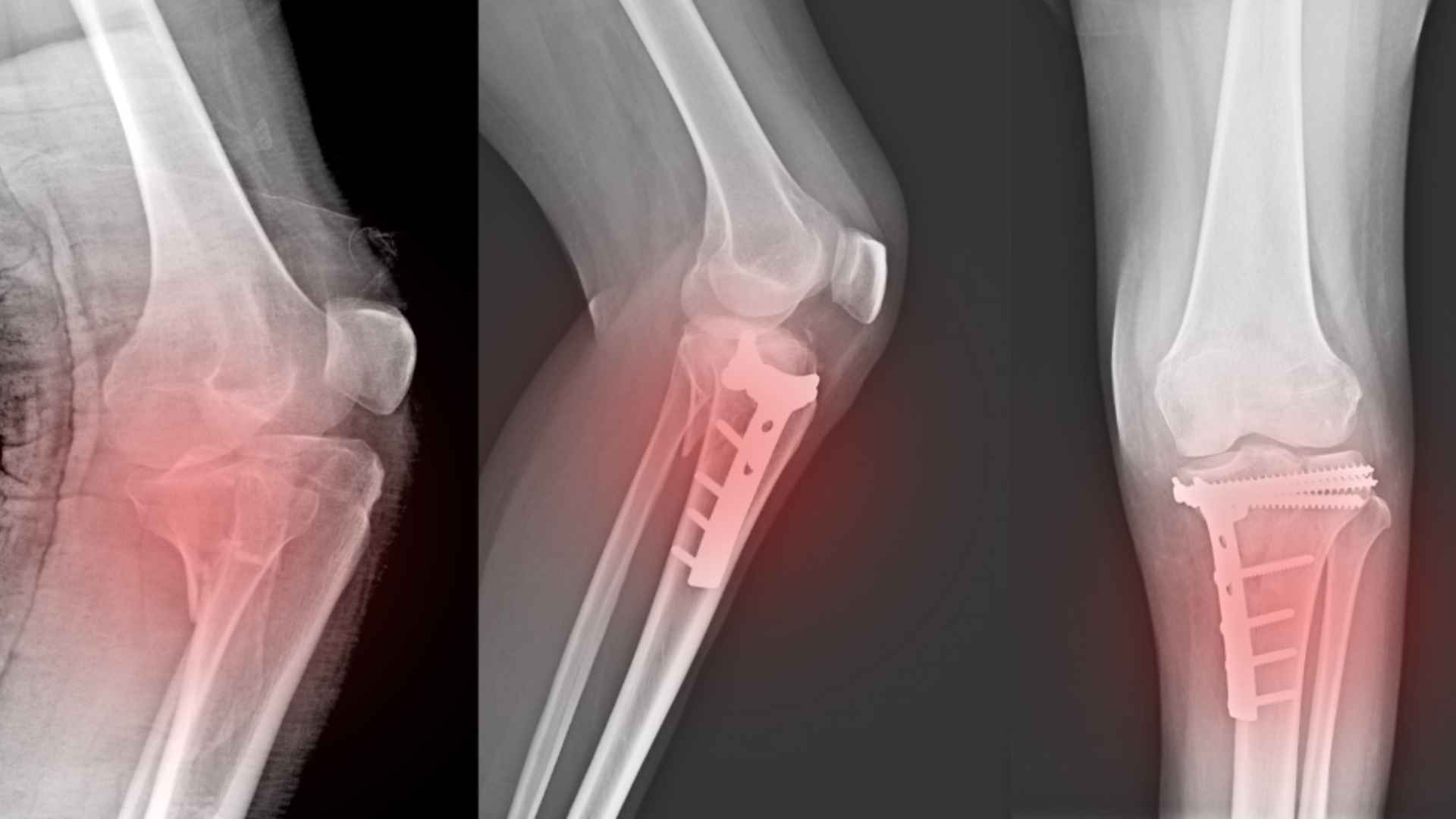
What Is a Fracture?
A fracture is a break or crack in a bone. Fractures can range from a tiny hairline crack to a complete break where the bone shatters into multiple pieces. They are one of the most common injuries treated in emergency departments, affecting people of all ages from children on playgrounds to seniors who suffer falls at home.
While fractures are rarely life-threatening on their own, they can cause severe pain, significant blood loss (especially with large bone fractures like the femur), and long-term complications if not treated properly. Knowing how to provide first aid for a suspected fracture can reduce pain, prevent further injury, and improve the person’s outcome.
Types of Fractures
Understanding the different types of fractures helps you assess the severity of an injury and provide appropriate first aid.
Closed fracture: The bone is broken but the skin remains intact. There may be significant swelling, bruising, and deformity, but no open wound at the fracture site. This is the most common type of fracture.
Open (compound) fracture: The broken bone pierces through the skin, creating an open wound. This type of fracture carries a high risk of infection and requires immediate medical attention. Do not attempt to push the bone back into place.
Stress fracture: A small crack in the bone caused by repetitive force or overuse, common in athletes and runners. Stress fractures may not be immediately obvious and can worsen over time if the person continues to put weight on the affected area.
Greenstick fracture: Common in children, this occurs when the bone bends and cracks on one side without breaking all the way through. Children’s bones are more flexible than adults’, which makes this pattern of injury unique to younger patients.
Hands-on first aid training makes all the difference. In a Standard First Aid course, you will practise splinting, bandaging, and assessing injuries under the guidance of a certified instructor. Find a course near you →
How to Recognize a Fracture
It can be difficult to tell whether an injury is a fracture, a sprain, or a dislocation without an X-ray. However, several signs suggest that a bone may be broken:
Pain that worsens with movement or pressure: Fracture pain is typically sharp and intense, especially when the injured area is touched or moved. The person may guard the injured area and resist any attempts to examine it.
Swelling and bruising: The area around the fracture will swell rapidly, and bruising may develop within hours. The swelling is caused by bleeding from the broken bone and surrounding damaged tissue.
Deformity: The limb may appear bent at an unnatural angle, shortened, or rotated compared to the other side. Any visible deformity is a strong indicator of a fracture.
Inability to use the injured part: The person may be unable to bear weight on an injured leg, grip with an injured hand, or move the injured area at all.
Grinding or crunching sensation: Called crepitus, this grating sound or feeling occurs when broken bone ends rub against each other. Do not deliberately test for this, as it causes additional pain and can worsen the injury.
Numbness or tingling: If the fracture is pressing on or has damaged a nerve, the person may experience numbness, tingling, or loss of sensation below the fracture site.
First Aid for Fractures: Step-by-Step
Step 1: Keep the Person Still
Tell the person not to move the injured area. Movement can cause the broken bone ends to shift, which can damage surrounding blood vessels, nerves, and muscles. Help the person get into a comfortable position that does not require moving the injured limb.
Step 2: Call for Medical Help
For suspected fractures of large bones (femur, pelvis, spine), open fractures, or any fracture that involves severe pain, deformity, or numbness, call 911. For smaller fractures (fingers, toes, wrist), the person may be able to go to an urgent care clinic or emergency department by car, but they should not drive themselves.
Step 3: Control Bleeding (Open Fractures)
If the fracture has broken through the skin, control bleeding by applying gentle pressure around the wound — not directly on the protruding bone. Cover the wound with a sterile dressing to reduce the risk of infection. Never try to realign the bone or push it back under the skin.
Step 4: Immobilize the Injury
The goal of immobilization is to prevent the broken bone from moving, which reduces pain and prevents further damage. If you have access to a commercial splint, use it according to your training. If not, you can improvise a splint using rigid materials such as a rolled-up magazine, a piece of wood, an umbrella, or even a pillow secured with tape or cloth strips.
When applying a splint, immobilize the joint above and below the fracture. For example, if the forearm is broken, the splint should extend from above the elbow to below the wrist. Pad the splint with soft material to prevent pressure sores, and secure it firmly but not so tight that it cuts off circulation. Check the fingers or toes below the splint regularly for color, warmth, and sensation.
Step 5: Apply Ice and Elevate
Apply a cold pack wrapped in a cloth to the injured area for 20 minutes at a time to reduce swelling and pain. Never apply ice directly to the skin. If possible, elevate the injured limb above the level of the heart to help minimize swelling.
Step 6: Treat for Shock
Fractures of large bones like the femur can cause significant internal bleeding and lead to shock. Signs of shock include pale and clammy skin, rapid breathing, weakness, and confusion. If you suspect shock, have the person lie down with their legs elevated slightly, cover them with a blanket to maintain body temperature, and monitor them closely until help arrives.
Special Situations
Suspected Spinal Fracture
If you suspect a fracture of the spine or neck — for example, after a fall from height, a diving accident, or a car crash — do not move the person unless they are in immediate danger. Moving someone with a spinal fracture can cause permanent paralysis. Keep the person’s head and neck in the position you found them, place your hands on either side of their head to prevent movement, and wait for paramedics to arrive. For more on spinal injuries and emergency first aid training, check our course options.
Pelvic Fracture
Pelvic fractures are serious injuries that can cause life-threatening internal bleeding. If you suspect a pelvic fracture — typically after a high-energy impact like a car accident or fall from height — do not move the person, do not ask them to stand, and call 911 immediately. Keep the person warm and monitor for signs of shock while waiting for emergency services.
When to Go to the Emergency Room
Seek emergency medical care for any fracture that involves visible deformity or bone protruding through the skin, numbness or loss of circulation below the injury, inability to move the affected limb, suspected fracture of the spine, pelvis, hip, or femur, or an injury accompanied by heavy bleeding. For fractures of smaller bones such as fingers or toes with minimal deformity, an urgent care visit within a few hours is usually appropriate.
Preventing Fractures
Many fractures are preventable. For older adults, fall prevention strategies such as removing tripping hazards, installing grab bars, maintaining good lighting, and staying physically active to preserve balance and bone density can significantly reduce fracture risk. For athletes, proper warm-up routines, appropriate protective equipment, and gradual increases in training intensity help prevent both acute fractures and stress fractures.
For children, supervision during play, age-appropriate sports equipment, and teaching safe practices on playgrounds and trampolines can reduce the likelihood of fractures. Ensuring adequate calcium and vitamin D intake throughout life supports bone health and resilience.
Learn First Aid at Coast2Coast
Fracture management, splinting, sling application, and shock treatment are all covered in our Standard First Aid and CPR courses. At Coast2Coast in Richmond Hill, Guelph, Newmarket, Windsor, and many more locations, you will get hands-on practice with real splinting and bandaging techniques so you know exactly what to do when an injury happens.
Register for CPR or First Aid Training
Register today for a CPR or First Aid training course at one of our 30+ locations across Canada and the U.S. Check out our facilities and book your spot now.
About the Author
Ashkon Pourheidary, B.Sc. (Hons) — Co-Founder, Coast2Coast First Aid & Aquatics
Ashkon has been a certified First Aid and CPR instructor since 2011 and an Instructor Trainer since 2013. He is also a certified Emergency Medical Responder (EMR) instructor, Psychological First Aid instructor, and BLS (Basic Life Support) instructor. Ashkon graduated with honours with a Bachelor of Science in Neuroscience from the University of Toronto in 2016. As co-founder of Coast2Coast First Aid & Aquatics, he has helped grow the organization to over 30 locations across Canada and into the United States. Ashkon has served on the First Aid Council for the Canadian Red Cross. He spends his time coaching the team of over 100 instructors at Coast2Coast to ensure that students training at Coast2Coast locations receive the best training experience. Connect on LinkedIn