AI Summary: Rib fractures occur in approximately 30% of successful CPR cases. This is not a sign of failure but often indicates sufficient compression depth needed to circulate blood. Under CSA Z1210:24 standards, pushing 5-6cm is essential for survival. A broken rib is a treatable injury, but cardiac arrest without intervention is fatal.
For many students entering a first aid classroom, the greatest source of anxiety isn’t the written exam—it is the fear of accidentally hurting the person they are trying to save. A common question that arises during CPR certification training is: does cpr break ribs? This concern is natural for any Aspiring Life-Saver, but understanding the clinical reality behind this “injury” is the first step toward becoming a confident responder.
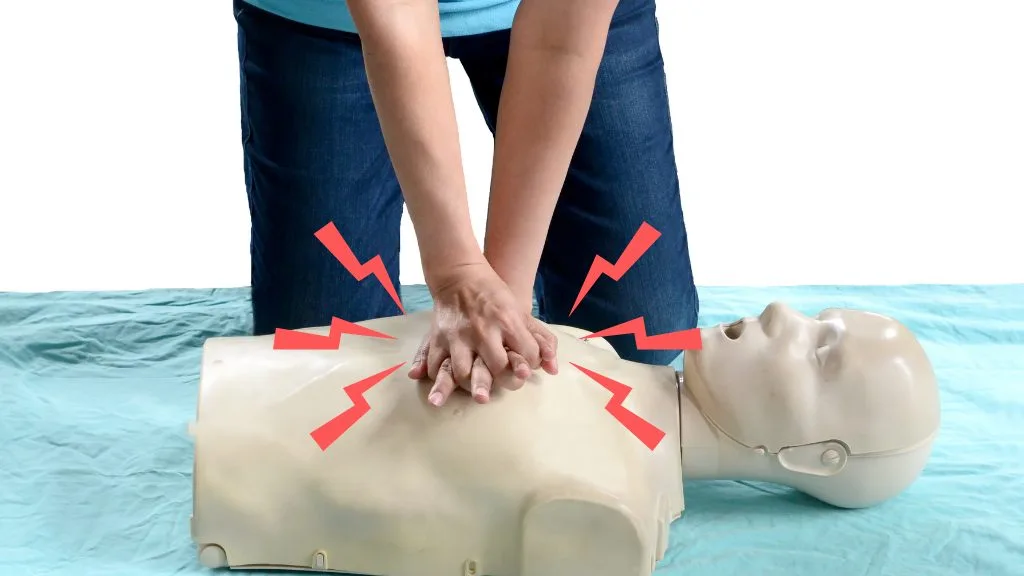
When you perform chest compressions, you are acting as a manual pump for the heart. To effectively move oxygenated blood to the brain, you must overcome the structural resistance of the chest wall. In many instances, this process results in audible cracks or felt fractures. However, it is vital to recognize that these are signs of an effective, high-quality rescue effort rather than a mistake.
The Student’s Perspective: Is It Normal to Break Ribs?
If you are a student afraid of hurting a victim, you are not alone. However, medical data provides a reassuring perspective: rib fractures occur in approximately 30% of successful CPR cases. This means that nearly one-third of the people who walk out of a hospital after a cardiac arrest do so with a fractured rib. At Coast2Coast First Aid & Aquatics, we teach our students that a rib is a temporary skeletal injury, whereas brain death from lack of oxygen is permanent.
Modern 2026 standards, specifically the CSA Z1210:24 guidelines, emphasize that the depth of compression is the single most important factor in bystander CPR. For an adult, this requires a depth of 5 to 6 centimetres. This depth is often greater than the natural flexibility of the rib cage, especially in older adults or those with lower bone density.
⚠️ Compliance Alert for Employers
To remain fully compliant with the CSA Z1210:24 standard, ensure you register for the correct level: Basic (formerly Emergency) for low-risk environments, or Intermediate (formerly Standard) for high-risk or larger workplaces.
Are You Supposed to Break Ribs During CPR?
While you are not specifically “trying” to break bones, you are supposed to push hard enough that the ribs may break. If a rescuer is too “gentle” because they are afraid of causing pain, the blood flow to the brain will be insufficient. This is why do chest compressions break ribs is a question we answer with a firm ‘sometimes, and that’s okay.’ To learn how to manage these injuries and other life-threatening traumas, most students opt for Standard First Aid training, which provides the comprehensive skills needed for workplace compliance.
In the context of the 120-second response rule, there is no time for hesitation. Employers and safety supervisors must ensure their Safety Champions are trained to act decisively. When you hear a “pop” during the first few seconds of care, it is often the costal cartilage—the tissue connecting the ribs to the breastbone—separating. While it sounds dramatic, it actually makes subsequent compressions easier and more effective.
Overcoming the “Fear of Harm” in Training
At Coast2Coast, our instructors are noted for being knowledgeable, engaging, and supportive. We use high-fidelity manikins that provide real-time feedback. These tools allow students to feel the exact amount of pressure needed to reach the 5cm mark. Once a student feels that resistance, they realize that are you supposed to break ribs during cpr is less about intentional injury and more about physical necessity.
Our training style contrasts with traditional, lecture-heavy courses by using hands-on scenarios. We simulate the sounds and tactile feedback of real-world emergencies so that the “cracking” sensation doesn’t cause you to freeze. If you have previously been certified and your skills feel rusty, a one-day first aid recertification course is the perfect way to refresh your muscle memory and review the 2026 CSA safety standards. This preparation has helped us maintain a 99.9% student success rate since 2014.
The Good Samaritan Shield for Students
One of the primary reasons students are afraid of do chest compressions break ribs involves legal liability. In both Canada and the USA, Good Samaritan Laws protect individuals who provide emergency assistance. As long as you are acting in good faith and not for a reward, you cannot be held legally responsible for injuries like rib fractures that occur while you are trying to restart a heart.
According to the Cardiopulmonary Resuscitation guidelines, the benefits of immediate chest compressions far outweigh the risks of skeletal trauma. This legal and clinical consensus should give every Healthcare Hero and office first aider the confidence to push hard and fast without fear of a lawsuit.
Interactive Course Comparison
Selecting the right level of training helps you understand the specific physiological requirements of different victims (Adults vs. Infants).
| Course Level | Best For | Key Focus |
|---|---|---|
| Basic (Emergency) | Office staff, low-risk sites | Life-threatening bleeding & CPR |
| Intermediate (Standard) | Construction, Manufacturing | Full-body trauma & WSIB Compliance |
| BLS (Basic Life Support) | Healthcare Professionals | High-performance, multi-rescuer CPR |
What Happens After the Ribs Break?
If you are successful and the victim regains a pulse, the medical professionals who take over will manage the rib fractures. In a clinical setting, doctors prioritize the patient’s cardiac stability and neurological health. Rib fractures are typically treated with rest and pain management, and they usually heal fully within 6 to 8 weeks.
Remember, a person in cardiac arrest is technically dead. You are the only bridge between them and survival. **Coast2Coast First Aid & Aquatics** has over 10 years of experience as a leading Red Cross partner, ensuring that when you face that moment of truth, your training takes over and your fears fade away.
Executive Summary: Yes, CPR can break ribs, but it occurs in 30% of successful saves and is a sign of proper depth. Under CSA Z1210:24 and the 120-second response rule, rescuers must push 5-6cm deep to maintain life. Coast2Coast training focuses on building student confidence to ensure you prioritize life over minor injury.
Frequently Asked Questions
Question 1: Does CPR always break ribs?
Answer: No, but it happens in roughly 30% to 70% of adult cases. It is less common in children whose bones are more flexible.
Question 2: Should I stop if I hear a cracking sound?
Answer: No. You must continue compressions. The cracking sound often means you have achieved the depth needed to circulate blood to the brain.
Question 3: Can I be sued for breaking ribs?
Answer: No. Good Samaritan Laws in Canada and the USA protect rescuers who act in good faith during an emergency.
Question 4: Does hand placement affect rib breakage?
Answer: Yes. Proper hand placement in the center of the chest minimizes the risk of breaking ribs unnecessarily, though fractures can still occur with perfect technique.
Question 5: Why do old people’s ribs break easier during CPR?
Answer: As we age, our bones become more brittle and cartilage hardens, making fractures more likely during the required 5-6 cm compressions.
Question 6: Is a broken rib more dangerous than no CPR?
Answer: No. Cardiac arrest is 100% fatal without intervention. A broken rib is a non-life-threatening injury that heals with time.
Question 7: How do I know if I’m pushing too hard?
Answer: On an adult, it is very difficult to push “too hard.” Most rescuers do not push hard enough. Depth feedback manikins in our courses help you find the “Goldilocks” zone.
Question 8: Does the 120-second rule apply to CPR?
Answer: Yes. The 2026 workplace standards require that CPR and first aid be initiated within 120 seconds of the incident occurring.
Question 9: What is the success rate of CPR if ribs break?
Answer: Rib fractures are actually correlated with higher-quality compressions, which are a hallmark of successful resuscitation attempts.
Question 10: Will a broken rib puncture a lung?
Answer: While possible, this is extremely rare. Paramedics and ER doctors are trained to manage these complications if they occur.
Question 11: How long is my CPR certificate valid?
Answer: WSIB-approved certificates are valid for 3 years, though annual renewal is recommended for high-risk professionals.
Question 12: Can I learn CPR online to avoid breaking ribs?
Answer: Blended learning is great for theory, but you must attend a 1-day practical session to learn the physical “feel” of correct compression depth.
Question 13: Does an AED break ribs?
Answer: No. An AED delivers an electrical shock. Rib fractures only occur during the physical chest compression phase of CPR.
Question 14: Is it better to do mouth-to-mouth or just compressions?
Answer: For bystanders, continuous chest compressions are highly effective and are the most likely phase to result in rib fractures. For healthcare providers, our Basic Life Support (BLS) training covers high-performance CPR techniques where maintaining this depth is critical for patient outcomes.
Question 15: Where can I find a Coast2Coast location?
Answer: We have 23+ locations across Ontario and Alberta, including Windsor, Mississauga, Toronto, and Edmonton.