Why Sports Injury First Aid Matters
Sports injuries are an everyday reality for athletes at every level — from children in recreational leagues to adults playing pickup basketball to elite competitors. According to public health statistics, millions of sports-related injuries are treated in emergency departments across North America each year. The most common include sprains, strains, fractures, dislocations, and concussions.
Knowing how to assess and provide first aid for sports injuries is essential for coaches, parents, athletic trainers, and fellow athletes. The first few minutes after an injury can determine how well a person recovers, whether the injury worsens, and how quickly they can return to the activities they love.
Common Sports Injuries and How to Treat Them
Ankle Sprains
Ankle sprains are the single most common sports injury. They occur when the foot rolls inward, stretching or tearing the ligaments on the outside of the ankle. You will notice rapid swelling, pain when bearing weight, and bruising that develops over hours.
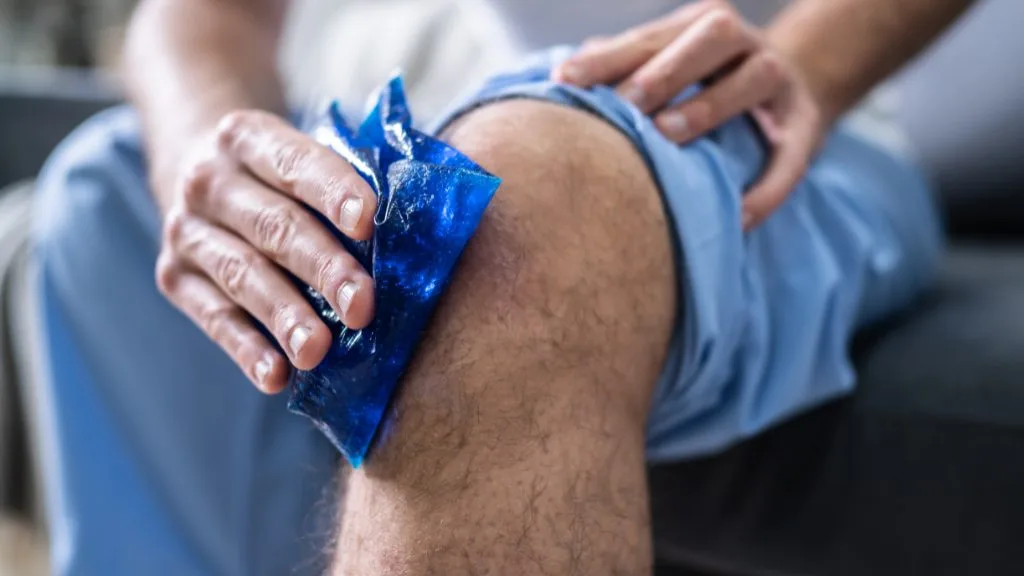
First aid for an ankle sprain follows the R.I.C.E. protocol: rest the ankle immediately, apply ice wrapped in a cloth for 20 minutes, compress with an elastic bandage, and elevate above heart level. The person should avoid walking on the injured ankle and seek medical evaluation if they cannot bear weight or if symptoms worsen.
Muscle Strains
Hamstring, quadriceps, and calf strains are common in sports that involve sprinting, jumping, and sudden changes of direction. The person typically feels a sudden sharp pain in the muscle, sometimes described as a “pop” or tearing sensation. Swelling and bruising may follow.
Stop the activity immediately. Apply ice and compression to the area, and have the person rest the injured muscle. Most mild strains heal with rest and gradual rehabilitation, but severe strains where the muscle is completely torn may require medical treatment.
Every Coach Should Be First Aid Certified
Whether you coach youth soccer or adult hockey, knowing first aid is part of being a responsible leader. Our courses cover sports-specific injury management, concussion protocols, and emergency response.
Knee Injuries
The knee is one of the most complex joints in the body and is vulnerable to a range of sports injuries including ACL tears, meniscus tears, and patellar dislocations. Knee injuries often occur during pivoting, cutting, landing from a jump, or direct impact.
If someone sustains a knee injury during sports, have them stop playing immediately. Do not allow them to walk on the injured leg if there is significant pain or instability. Apply ice and compression, keep the knee in a comfortable position (usually slightly bent), and arrange for medical evaluation. Knee injuries often require imaging (X-ray or MRI) to determine the extent of damage.
Dislocations
A dislocation occurs when the bones of a joint are forced out of their normal alignment. Shoulder dislocations are common in contact sports, while finger dislocations frequently occur in ball sports like basketball and volleyball.
A dislocated joint appears visibly deformed and is extremely painful. The person will be unable to move the joint normally. First aid for a dislocation involves immobilizing the joint in the position you find it — do not attempt to push the bone back into place, as this can cause nerve and blood vessel damage. Apply ice, support the joint with a sling or splint, and transport the person to the emergency room.
Concussions
Concussions are particularly prevalent in contact and collision sports. Any athlete who takes a blow to the head or body and shows signs of confusion, headache, dizziness, balance problems, or altered consciousness should be removed from play immediately and not allowed to return until cleared by a healthcare provider. For a comprehensive guide on concussion recognition and first aid, see our detailed article.
Fractures
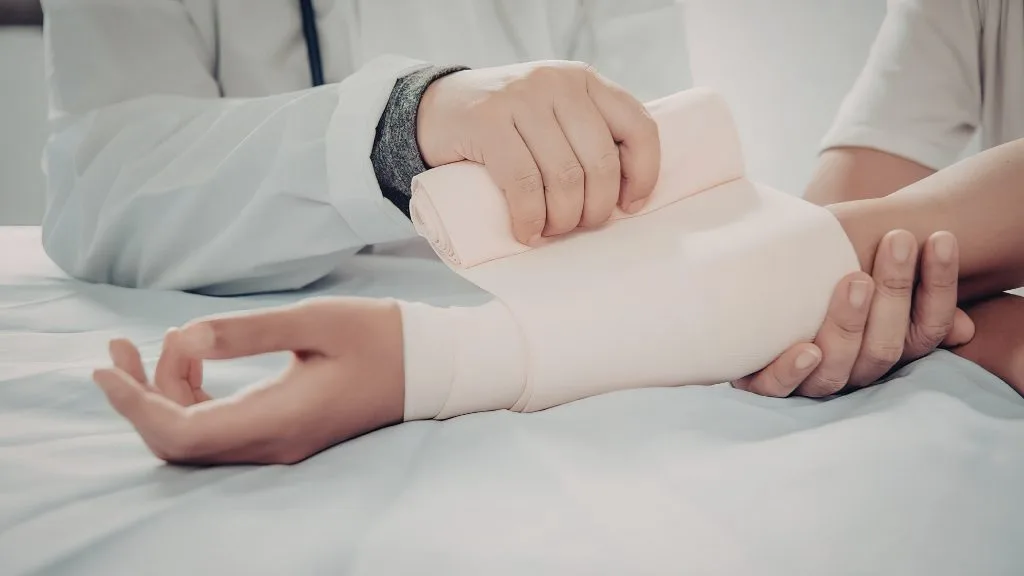
Fractures can occur in virtually any sport but are most common in high-impact and collision activities. A suspected fracture should be immobilized with a splint, and the person should be transported for X-rays. Open fractures — where bone protrudes through the skin — are medical emergencies requiring immediate 911 activation.
Heat-Related Illness in Sports
Athletes training or competing in hot weather are at risk for heat exhaustion and heat stroke. Heat exhaustion symptoms include heavy sweating, weakness, nausea, and dizziness. If recognized early, it can be treated by moving the person to a cool area, removing excess clothing, applying cool water, and having them drink fluids.
Heat stroke is a life-threatening escalation where the body’s temperature regulation fails. The person may stop sweating, become confused, or lose consciousness. Heat stroke requires immediate 911 activation and aggressive cooling while waiting for paramedics.
Building a Sports First Aid Kit
Every team, gym, and sports facility should have a well-stocked first aid kit readily accessible. A comprehensive sports first aid kit should include instant cold packs, elastic bandages of various sizes, adhesive bandages and gauze, athletic tape, a SAM splint or similar malleable splint, scissors and tweezers, antiseptic wipes, gloves, a CPR pocket mask, and a first aid manual.
The kit should be checked and restocked regularly. Assign someone on the team — a coach, manager, or designated first aider — to be responsible for maintaining the kit and ensuring it is brought to every practice and game.
The Role of First Aid Training in Sports
Many sports organizations now require or strongly recommend that coaches hold a current first aid certification. This makes sense — coaches are almost always the first adults on scene when an athlete is injured. A certified coach can assess injuries accurately, provide appropriate first aid, decide when an injury requires medical evaluation, and manage the situation calmly and effectively.
Parents of young athletes also benefit from first aid training. Knowing what to do when your child is injured — whether at a game, practice, or in the backyard — reduces anxiety for both you and your child and ensures the best possible outcome.
Train with Coast2Coast
Our Standard First Aid and CPR courses cover everything from sprains and strains to concussions to CPR and AED use. With over 30 locations including Regina, Halifax, Peterborough, and Los Angeles, finding a course near you is easy.
Register for CPR or First Aid Training
Register today for a CPR or First Aid training course at one of our 30+ locations across Canada and the U.S. Check out our facilities and book your spot now.
About the Author
Ashkon Pourheidary, B.Sc. (Hons) — Co-Founder, Coast2Coast First Aid & Aquatics
Ashkon has been a certified First Aid and CPR instructor since 2011 and an Instructor Trainer since 2013. He is also a certified Emergency Medical Responder (EMR) instructor, Psychological First Aid instructor, and BLS (Basic Life Support) instructor. Ashkon graduated with honours with a Bachelor of Science in Neuroscience from the University of Toronto in 2016. As co-founder of Coast2Coast First Aid & Aquatics, he has helped grow the organization to over 30 locations across Canada and into the United States. Ashkon has served on the First Aid Council for the Canadian Red Cross. He spends his time coaching the team of over 100 instructors at Coast2Coast to ensure that students training at Coast2Coast locations receive the best training experience. Connect on LinkedIn