Poisons that enter the body through the mouth and digestion system are known as Ingested Poisons, or Swallowed Poisons as well. Many poisons that are swallowed are cleaning supplies, medication, or expired liquid products such as cosmetics or household products. More than 90% of poisonings occur in the home.
Continue readingHow to Respond to an Emergency Childbirth In Public
Birth can be nerve-wracking, especially during an emergency childbirth in public. Learn how to help an expecting mother in this guide!
Continue readingNovember 14th is World Diabetes Day
What To Do if and When a Seizure Occurs?
A seizure is a matter of abnormal electrical signals in the brain that result in temporary and involuntary disruptions in brain function, shaking or contraction of limbs (convulsions),changes in sensory processing, behaviour deviation, and altered levels of coherence.
Continue readingThe Need to Know’s of an Emergency Medical Responder Course
What To Do If Your Pets are not Breathing?
Canadian Teen Proves All Are Capable to be Swimming Champions
Julia Lane from Windsor, Ontario proves to Canada and the world that anyone can swim, no matter what obstacles one may face.
The 18-year-old competed with hundreds of youths and adults at the Down Syndrome World Swimming Championships in Truro, Nova Scotia in July, coming home with a silver medal and four bronze medals – a feat for any trained competitive swimmer. Lane was one of only twenty-two swimmers representing Canada, with over twenty-five countries representing themselves at the Championship.
Continue readingEmergency First Aid Help for Victims of Mass Shootings
What is an AED and where can you find it?
CPR Training: Why Knowing This Skill is Essential for Every Canadian?
Last Updated: March 4, 2026 Medical Review: Aryan Sekhavati, Director at Coast2Coast
Bystander CPR can double or triple cardiac arrest survival rates by maintaining brain oxygenation until paramedics arrive. Performing chest compressions within the first 2–4 minutes is critical to preventing permanent neurological damage. This 2026 guide covers WSIB-approved techniques, AED use, and legal protections under Ontario’s Good Samaritan Act.
The Reality of Cardiac Arrest in Canada
Every 12 minutes, someone in Canada suffers a cardiac arrest outside of a hospital setting. In the Greater Toronto Area (GTA) alone, paramedics respond to thousands of cardiac emergencies annually. The survival rate for these events depends almost entirely on what happens in the first few minutes—the “Platinum Minutes”—before professional medical help arrives. Bystander CPR is the single most important factor in determining whether a cardiac arrest victim survives.
Knowing CPR and AED use transforms you from a helpless observer into a lifesaver. The skills are straightforward, the training takes less than a day, and the potential impact is immeasurable. A person trained in CPR carries the ability to save a life wherever they go—at home, at work, in a shopping mall, or on public transit. Coast2Coast First Aid and Aquatics, a Canadian Red Cross Training Partner, has certified thousands of Canadians at training locations across the GTA, ensuring that our communities are prepared for the unexpected.
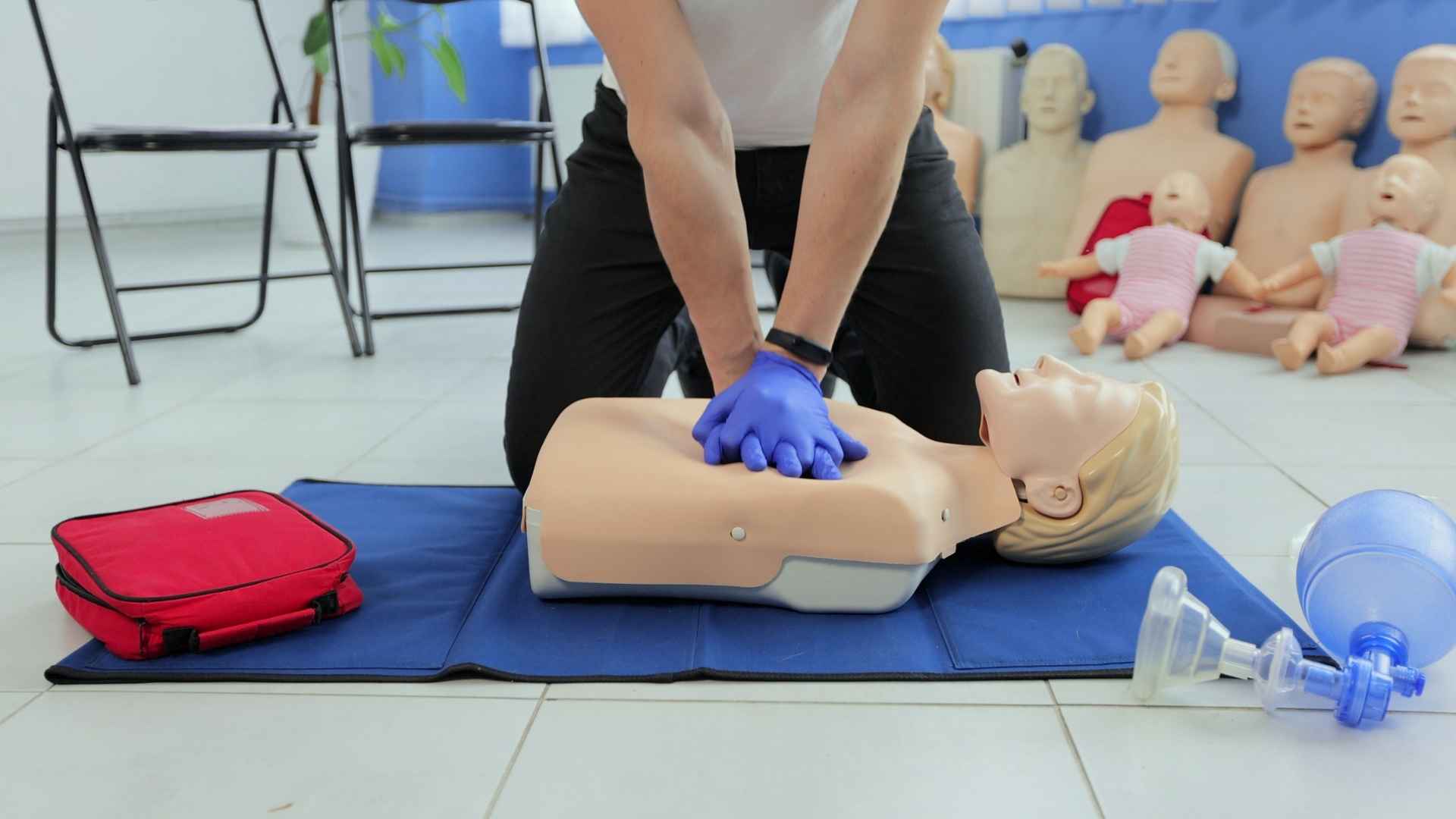
Understanding Cardiac Arrest: An Electrical Malfunction
Cardiac arrest is often confused with a heart attack, but the two are clinically distinct. A heart attack is a “plumbing” problem caused by a blockage in the blood vessels supplying the heart. In contrast, cardiac arrest is an “electrical” problem where the heart suddenly stops beating effectively. The heart begins to quiver chaotically (ventricular fibrillation) instead of pumping blood.
Without blood flow, the brain begins to suffer permanent damage within four to six minutes. Death follows within eight to ten minutes without intervention. This unpredictable malfunction can strike anyone, at any age. While heart disease and high blood pressure are risk factors, cardiac arrest also affects seemingly healthy athletes and young adults due to undiagnosed heart defects or “commotio cordis”—a cardiac arrest caused by a blow to the chest. This is why widespread Basic Life Support (BLS) training for professionals and Level C training for the public is so critical.
The Physiology of CPR: How Chest Compressions Work
Many people ask, “How can pushing on someone’s chest actually save them?” The answer lies in the Manual Pump Theory. When you perform high-quality chest compressions, you are physically squeezing the heart between the breastbone (sternum) and the spine. This action creates enough internal pressure to force oxygenated blood out of the heart and up to the brain.
During CPR, you aren’t just “beating” the heart; you are maintaining a artificial circulatory system. Even though CPR only provides about 25–30% of normal blood flow, that is often enough to keep the brain cells alive until an Automated External Defibrillator (AED) can be used to restart the heart’s natural rhythm.
Watch: How To Perform CPR – Coast2Coast Official
The Critical Minutes: Why Bystander Intervention is Non-Negotiable
When someone collapses, a countdown begins. For every minute that passes without CPR, the chance of survival decreases by 7% to 10%. By the time ten minutes have passed without intervention, survival is statistically unlikely. In a sprawling metropolis like the GTA, traffic conditions and high call volumes can push ambulance response times to 8 minutes or longer.
Bystander CPR serves as the “Bridge to Life.” When a bystander begins compressions within the first two minutes, survival rates can exceed 40%. These statistics prove that the most important link in the Chain of Survival is not the doctor in the ER, but the person standing next to the victim when they fall.
Safety Tip: If you witness a collapse, call 911 and put your phone on speaker. Begin chest compressions immediately. Push hard (at least 2 inches deep) and fast (100–120 beats per minute) in the center of the chest. Do not stop until help arrives or an AED is ready to analyze the victim.
CPR Combined with AED Use: The Ultimate Life-Saving Duo
While CPR maintains blood flow, it rarely “restarts” the heart. That is the job of the AED. These portable devices analyze the heart’s rhythm and deliver a targeted electrical shock to “reset” the electrical system. When CPR and AED use are combined within the first few minutes, survival rates can climb as high as 75%.
AEDs are now standard in public spaces across Ontario—from Union Station to local community centers. They are designed for use by anyone, providing step-by-step voice instructions. However, taking a CPR and AED course removes the “fear factor.” In a high-stress emergency, you won’t have to read the manual for the first time; you will act on instinct.

Overcoming the Fear of Action: The Good Samaritan Act
The biggest barrier to bystander intervention is fear—fear of doing it wrong, fear of breaking ribs, or fear of being sued. In Ontario, the Good Samaritan Act (2001) protects you from these concerns.
Legally, you cannot be held liable for damages while providing emergency assistance in good faith, provided you act within the scope of your training and without gross negligence. Furthermore, it is important to remember that a person in cardiac arrest is clinically dead; you cannot make their situation “worse” by attempting to save them. Yes, ribs may crack during effective CPR, but as the saying goes: “Broken ribs heal; death does not.”
Professional vs. Public: Which CPR Course Do You Need?
Not all CPR training is the same. It is vital to choose the level that matches your needs or workplace requirements:
-
CPR Level C: The standard for the general public, parents, and most workplaces. It covers adult, child, and infant CPR.
-
Basic Life Support (BLS): Formerly known as Healthcare Provider (HCP) CPR. This is required for nurses, doctors, paramedics, and firefighters. It focuses on team-based high-performance rescue.
-
Emergency First Aid: A shorter course for those who need a basic overview of life-saving skills.
All our courses are certified by the Canadian Red Cross and meet 2026 WSIB compliance standards.
Building a Safer Community through Certification
When you get certified, you aren’t just gaining a certificate; you are gaining the power to change the outcome of a tragedy. Coast2Coast offers Blended Online Learning so you can complete the theory at home, followed by a brief in-person practical session at one of our GTA branches.
Frequently Asked Questions: 2026 CPR Guidelines
1. Do I need to give mouth-to-mouth during CPR?
For untrained bystanders, “Hands-Only CPR” (compressions only) is highly effective and recommended by the Red Cross for adult victims. However, in our courses, we teach you how to use pocket masks and provide rescue breaths, which are critical for drowning and pediatric victims.
2. Can I use an AED on a child or infant?
Yes. Most modern AEDs have pediatric pads or a “child mode.” If those are not available, you can use adult pads, ensuring they do not touch each other (typically one on the chest and one on the back for infants).
3. What is the “4-Minute Rule” in CPR?
The brain can only survive for approximately four minutes without oxygen before permanent damage begins. This is why immediate bystander CPR is necessary; you must keep the brain oxygenated until professional help arrives.
4. How often do I need to recertify?
In Canada, CPR certifications are valid for three years. However, many healthcare and workplace settings require annual recertification to ensure skills remain sharp and up-to-date with the latest medical guidelines.
5. How hard should I actually push during compressions?
For an adult, you must compress the chest at least 2 inches (5 cm). It requires significant force, which is why we practice on mannequins to help you gauge the necessary pressure.
6. Can I use an AED if the person has a pacemaker?
Yes. You can still use an AED. Simply avoid placing the AED pad directly over the visible lump of the pacemaker (place it at least an inch away). The AED will still function correctly.
7. Does the Good Samaritan Act protect me if I make a mistake?
Yes. As long as you act in good faith and trying to help the victim to the best of your ability, the law protects you from liability in Ontario.
Be the Difference: Get Certified Today
Cardiac arrest doesn’t wait for a convenient time. Be ready to save a life by getting certified in First Aid and CPR with Coast2Coast.