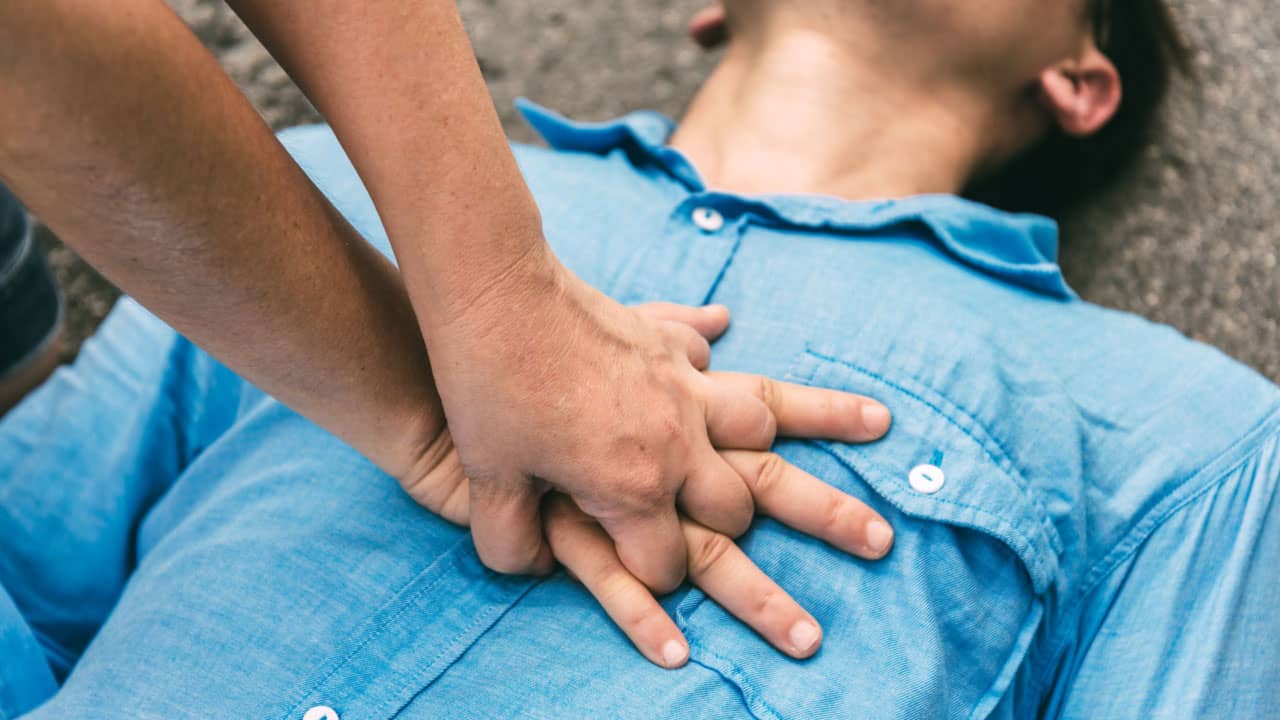
Do you know what the top 10 first aid emergencies are? We discuss the most important emergencies you should be prepared for.
Continue readingCompleting First Aid and CPR/AED Training in Toronto
Interested in First Aid and CPR/AED training in Toronto? Learn about different course levels and delivery methods for your training.
Continue readingWhat are the Different Levels of First Aid & CPR/AED?
You’re required to be First Aid and CPR/AED certified for your job, but do you know what the different levels of First Aid and CPR entail?
Continue readingHow Long is First Aid and CPR Valid in Ontario?
You’re interested in becoming First Aid and CPR certified, but how long is First Aid and CPR valid for in Ontario? Always keep your certificate up-to-date!
Continue reading7 Important Steps of CPR
If you come across someone who requires CPR, do you know how to help them? Follow these important steps of CPR and provide the victim with a fighting chance.
Continue readingWhy Don’t you Offer the CPR HCP Course?
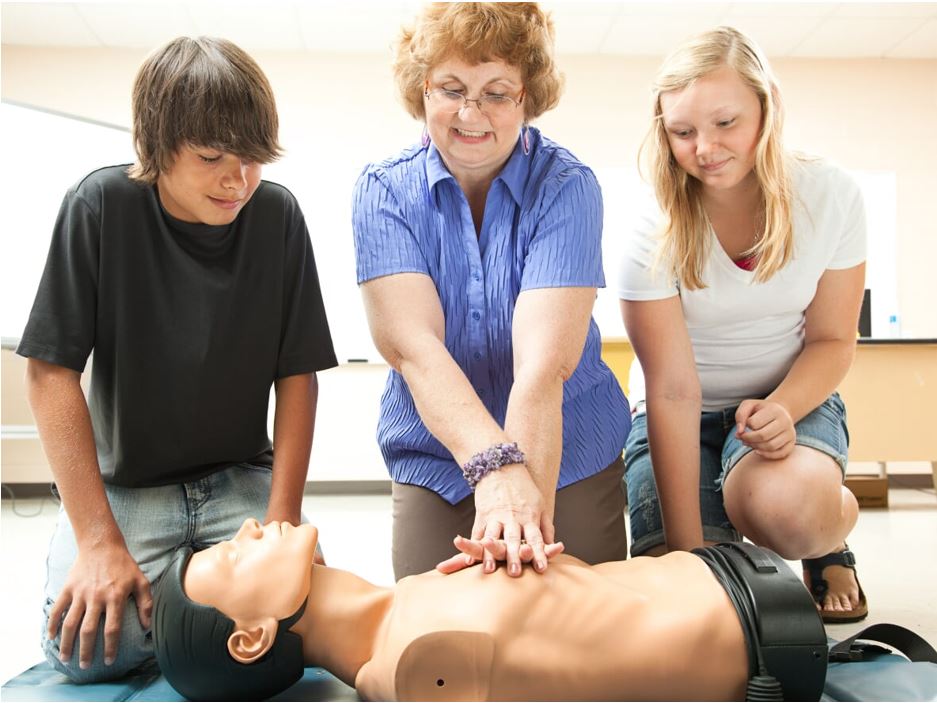
Should Children Learn CPR?
The story of two boys saving their grandma from death using CPR skills their mother taught them is an amazing feature, and further proves that even with just a little training, all can save lives no matter what age or size.
Continue readingWhat To Do If Your Pets are not Breathing?
CPR Training: Why Knowing This Skill is Essential for Every Canadian?
Last Updated: March 4, 2026 Medical Review: Aryan Sekhavati, Director at Coast2Coast
Bystander CPR can double or triple cardiac arrest survival rates by maintaining brain oxygenation until paramedics arrive. Performing chest compressions within the first 2–4 minutes is critical to preventing permanent neurological damage. This 2026 guide covers WSIB-approved techniques, AED use, and legal protections under Ontario’s Good Samaritan Act.
The Reality of Cardiac Arrest in Canada
Every 12 minutes, someone in Canada suffers a cardiac arrest outside of a hospital setting. In the Greater Toronto Area (GTA) alone, paramedics respond to thousands of cardiac emergencies annually. The survival rate for these events depends almost entirely on what happens in the first few minutes—the “Platinum Minutes”—before professional medical help arrives. Bystander CPR is the single most important factor in determining whether a cardiac arrest victim survives.
Knowing CPR and AED use transforms you from a helpless observer into a lifesaver. The skills are straightforward, the training takes less than a day, and the potential impact is immeasurable. A person trained in CPR carries the ability to save a life wherever they go—at home, at work, in a shopping mall, or on public transit. Coast2Coast First Aid and Aquatics, a Canadian Red Cross Training Partner, has certified thousands of Canadians at training locations across the GTA, ensuring that our communities are prepared for the unexpected.
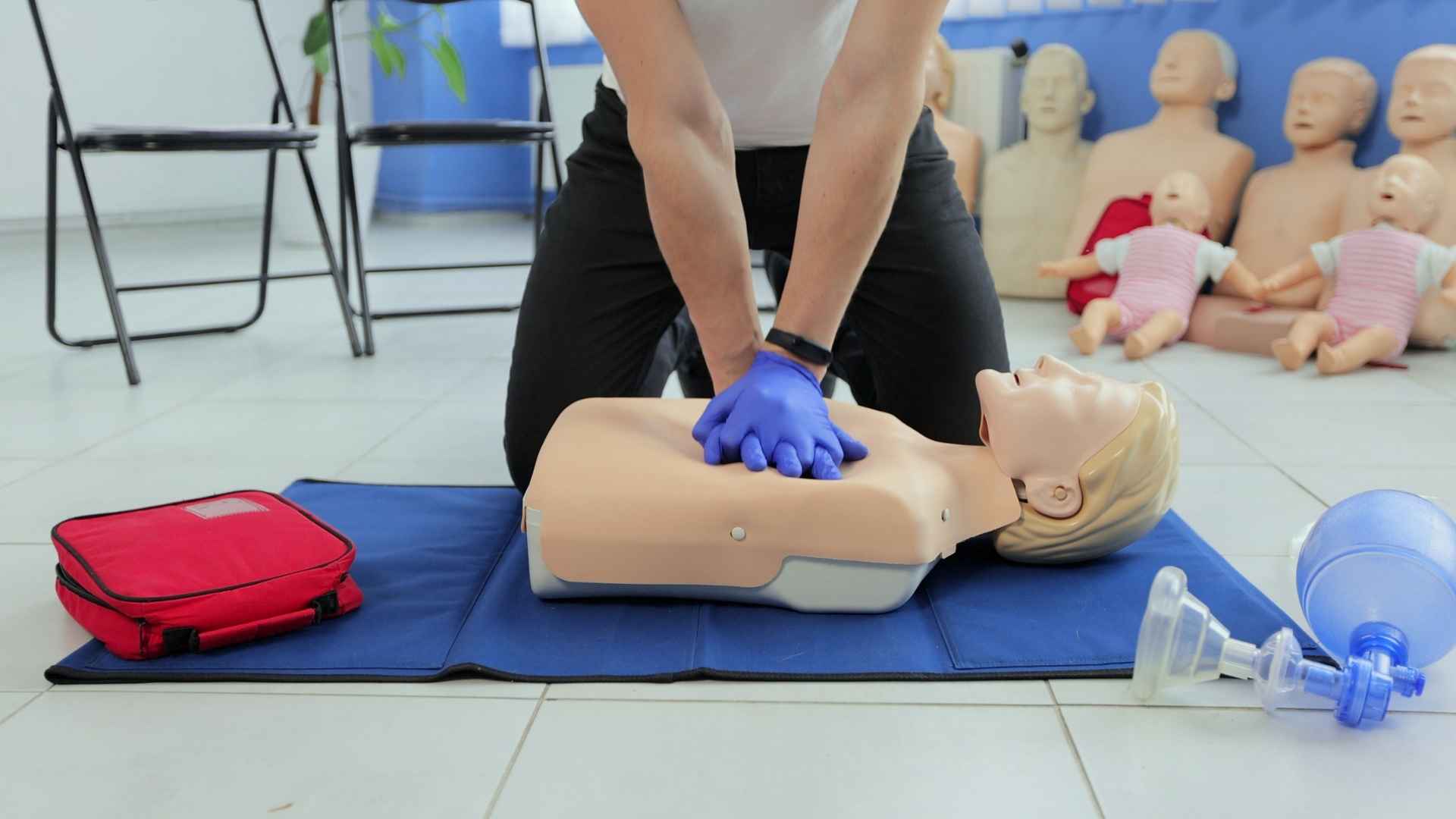
Understanding Cardiac Arrest: An Electrical Malfunction
Cardiac arrest is often confused with a heart attack, but the two are clinically distinct. A heart attack is a “plumbing” problem caused by a blockage in the blood vessels supplying the heart. In contrast, cardiac arrest is an “electrical” problem where the heart suddenly stops beating effectively. The heart begins to quiver chaotically (ventricular fibrillation) instead of pumping blood.
Without blood flow, the brain begins to suffer permanent damage within four to six minutes. Death follows within eight to ten minutes without intervention. This unpredictable malfunction can strike anyone, at any age. While heart disease and high blood pressure are risk factors, cardiac arrest also affects seemingly healthy athletes and young adults due to undiagnosed heart defects or “commotio cordis”—a cardiac arrest caused by a blow to the chest. This is why widespread Basic Life Support (BLS) training for professionals and Level C training for the public is so critical.
The Physiology of CPR: How Chest Compressions Work
Many people ask, “How can pushing on someone’s chest actually save them?” The answer lies in the Manual Pump Theory. When you perform high-quality chest compressions, you are physically squeezing the heart between the breastbone (sternum) and the spine. This action creates enough internal pressure to force oxygenated blood out of the heart and up to the brain.
During CPR, you aren’t just “beating” the heart; you are maintaining a artificial circulatory system. Even though CPR only provides about 25–30% of normal blood flow, that is often enough to keep the brain cells alive until an Automated External Defibrillator (AED) can be used to restart the heart’s natural rhythm.
Watch: How To Perform CPR – Coast2Coast Official
The Critical Minutes: Why Bystander Intervention is Non-Negotiable
When someone collapses, a countdown begins. For every minute that passes without CPR, the chance of survival decreases by 7% to 10%. By the time ten minutes have passed without intervention, survival is statistically unlikely. In a sprawling metropolis like the GTA, traffic conditions and high call volumes can push ambulance response times to 8 minutes or longer.
Bystander CPR serves as the “Bridge to Life.” When a bystander begins compressions within the first two minutes, survival rates can exceed 40%. These statistics prove that the most important link in the Chain of Survival is not the doctor in the ER, but the person standing next to the victim when they fall.
Safety Tip: If you witness a collapse, call 911 and put your phone on speaker. Begin chest compressions immediately. Push hard (at least 2 inches deep) and fast (100–120 beats per minute) in the center of the chest. Do not stop until help arrives or an AED is ready to analyze the victim.
CPR Combined with AED Use: The Ultimate Life-Saving Duo
While CPR maintains blood flow, it rarely “restarts” the heart. That is the job of the AED. These portable devices analyze the heart’s rhythm and deliver a targeted electrical shock to “reset” the electrical system. When CPR and AED use are combined within the first few minutes, survival rates can climb as high as 75%.
AEDs are now standard in public spaces across Ontario—from Union Station to local community centers. They are designed for use by anyone, providing step-by-step voice instructions. However, taking a CPR and AED course removes the “fear factor.” In a high-stress emergency, you won’t have to read the manual for the first time; you will act on instinct.

Overcoming the Fear of Action: The Good Samaritan Act
The biggest barrier to bystander intervention is fear—fear of doing it wrong, fear of breaking ribs, or fear of being sued. In Ontario, the Good Samaritan Act (2001) protects you from these concerns.
Legally, you cannot be held liable for damages while providing emergency assistance in good faith, provided you act within the scope of your training and without gross negligence. Furthermore, it is important to remember that a person in cardiac arrest is clinically dead; you cannot make their situation “worse” by attempting to save them. Yes, ribs may crack during effective CPR, but as the saying goes: “Broken ribs heal; death does not.”
Professional vs. Public: Which CPR Course Do You Need?
Not all CPR training is the same. It is vital to choose the level that matches your needs or workplace requirements:
-
CPR Level C: The standard for the general public, parents, and most workplaces. It covers adult, child, and infant CPR.
-
Basic Life Support (BLS): Formerly known as Healthcare Provider (HCP) CPR. This is required for nurses, doctors, paramedics, and firefighters. It focuses on team-based high-performance rescue.
-
Emergency First Aid: A shorter course for those who need a basic overview of life-saving skills.
All our courses are certified by the Canadian Red Cross and meet 2026 WSIB compliance standards.
Building a Safer Community through Certification
When you get certified, you aren’t just gaining a certificate; you are gaining the power to change the outcome of a tragedy. Coast2Coast offers Blended Online Learning so you can complete the theory at home, followed by a brief in-person practical session at one of our GTA branches.
Frequently Asked Questions: 2026 CPR Guidelines
1. Do I need to give mouth-to-mouth during CPR?
For untrained bystanders, “Hands-Only CPR” (compressions only) is highly effective and recommended by the Red Cross for adult victims. However, in our courses, we teach you how to use pocket masks and provide rescue breaths, which are critical for drowning and pediatric victims.
2. Can I use an AED on a child or infant?
Yes. Most modern AEDs have pediatric pads or a “child mode.” If those are not available, you can use adult pads, ensuring they do not touch each other (typically one on the chest and one on the back for infants).
3. What is the “4-Minute Rule” in CPR?
The brain can only survive for approximately four minutes without oxygen before permanent damage begins. This is why immediate bystander CPR is necessary; you must keep the brain oxygenated until professional help arrives.
4. How often do I need to recertify?
In Canada, CPR certifications are valid for three years. However, many healthcare and workplace settings require annual recertification to ensure skills remain sharp and up-to-date with the latest medical guidelines.
5. How hard should I actually push during compressions?
For an adult, you must compress the chest at least 2 inches (5 cm). It requires significant force, which is why we practice on mannequins to help you gauge the necessary pressure.
6. Can I use an AED if the person has a pacemaker?
Yes. You can still use an AED. Simply avoid placing the AED pad directly over the visible lump of the pacemaker (place it at least an inch away). The AED will still function correctly.
7. Does the Good Samaritan Act protect me if I make a mistake?
Yes. As long as you act in good faith and trying to help the victim to the best of your ability, the law protects you from liability in Ontario.
Be the Difference: Get Certified Today
Cardiac arrest doesn’t wait for a convenient time. Be ready to save a life by getting certified in First Aid and CPR with Coast2Coast.
Are You Ready to Act? What to Expect in Your Toronto CPR Course
Reviewed by: Aryan Sekhavati, Director at Coast2Coast
The Quick Take: Succeeding in a Toronto CPR course in 2026 requires mastering the CSA Z1210:24 standards and high-performance resuscitation techniques. Whether you are a healthcare provider seeking BLS/ACLS or a community responder aiming for Level C, your training focuses on the “Platinum Minutes” of an emergency. Learn why immediate recognition and the use of feedback-enabled manikins are the gold standards for survival in the GTA.
Are You Ready to Act? What to Expect in Your Toronto CPR Course
Toronto is a city of nearly three million people, and with that population comes the reality that cardiac emergencies, choking incidents, and other life-threatening situations occur every single day. Whether you are navigating the Financial District, commuting on the TTC, or coaching youth sports in Scarborough, the ability to perform CPR is the ultimate urban survival skill. In an emergency, knowing CPR can save someone’s life by providing immediate care until professional help arrives.
Taking a CPR course in Toronto is one of the most valuable investments you can make in your personal preparedness. These courses teach you how to recognize cardiac arrest, perform high-quality chest compressions, deliver rescue breaths, and use an automated external defibrillator (AED). At Coast2Coast, we’ve updated our curriculum to reflect the fast-paced nature of the GTA, ensuring you have the hands-on, scenario-based training needed to build real confidence.
Understanding Cardiac Arrest: The Need for Speed
Cardiac arrest is a sudden, life-threatening emergency where the heart unexpectedly stops beating, cutting off blood flow and oxygen to the brain and vital organs. This can be triggered by heart attack, stroke, severe trauma, or electrical shock. Immediate recognition is essential—every minute without basic life support (BLS) reduces survival chances by about 10%. This is why healthcare providers and trained community responders are the most vital link in the survival chain.
For healthcare professionals, Advanced Cardiovascular Life Support (ACLS) and Pediatric Advanced Life Support (PALS) provide the specialized skills needed for complex emergencies. However, for the general public, the foundation of every “save” starts with high-quality Basic Life Support. In every Coast2Coast course, we emphasize rapid recognition and effective communication because, in a cardiac emergency, every second counts toward survival.
The Science of the Save: What Happens During CPR?
In 2026, CPR is recognized as a clinical “bridge” to survival. When a person experiences cardiopulmonary arrest, the brain begins to suffer irreversible damage within four to six minutes. CPR works by manually pumping the heart through chest compressions, forcing oxygenated blood to circulate to vital organs. While CPR alone may not restart the heart, it maintains blood flow and buys precious time for an AED or paramedics to arrive. We focus heavily on Chest Compression Fraction (CCF)—keeping your hands on the chest at least 80% of the time to maintain critical blood pressure.
High-Fidelity Training: The 2026 Tech Difference
Modern training has moved away from rubber dolls to High-Fidelity Feedback Manikins. These trainers use sensors to provide real-time data on your depth (at least 2 inches) and rate (100-120 bpm). This data-driven approach builds Correct Muscle Memory, making you 50% more likely to deliver effective compressions in a high-stress scenario. We ensure every student masters airway management and trauma response using these advanced tools at our Toronto training locations.
The “Vertical Response” Challenge: Toronto Skyscrapers
If you work in a high-rise in the Financial District or live in a CityPlace condo, you face the “Vertical Delay.” Reaching the 40th floor adds 5–8 minutes to emergency response times. Our training covers urban logistics, such as coordinating “Elevator Recall” with security and locating AEDs in lobbies. In a skyscraper, you aren’t just a bystander; you are the primary medical responder until help navigates the building’s architecture.
Benefits of CPR Training for Your Community
CPR training is more than a certification—it’s an investment in community safety. Organizations like the Stroke Foundation highlight the importance of widespread education in improving survival rates. By learning CPR, you gain the confidence to respond to cardiac arrest, stroke, and trauma at home or in the workplace. Successful completion empowers you to provide care that potentially saves a life, joining a foundation of responders committed to quality intervention.
Types of CPR Courses Available in Toronto
The Canadian Red Cross offers several levels to meet professional and personal needs:
- CPR Level A: Focuses on adult CPR and choking. Ideal for personal preparedness.
- CPR Level C: Our most popular choice. Covers adults, children, and infants. Required for most Ontario employers.
- Basic Life Support (BLS): Designed for nurses, physicians, and paramedics. Includes team-based resuscitation. Explore our BLS courses in Toronto.
Legal Realities: The Good Samaritan Act & WSIB
In Ontario, the Good Samaritan Act provides legal protection to those helping in good faith within their training scope. Professionally, WSIB Regulation 1101 mandates certified first aiders on staff. The 2026 shift to CSA Z1210:24 standards ensures your training meets the latest international scientific evidence for emergency cardiovascular care. Whether you choose in-person or blended first aid learning, your certificate is a career-boosting asset.
Get CPR Certified in Toronto Today
Join thousands of Torontonians who have earned their certification with Coast2Coast. Choose from flexible dates at convenient GTA locations.
Frequently Asked Questions About Toronto CPR Training
1. Do I need any prior experience to take a CPR course?
No prior experience is required. Courses are designed for complete beginners and your instructor will guide you through every skill from the basics.
2. How much does a CPR course cost in Toronto?
Fees vary by level (A, C, or BLS). You can find current pricing on our registration page.
3. Can I take a CPR course online?
You can complete the theory via blended learning online, but the hands-on skills evaluation must be done in person for official certification.
4. What should I bring to my CPR course?
Wear comfortable clothes, bring photo ID, and your confirmation email. All training equipment is provided by Coast2Coast.
5. How do I renew my expiring certificate?
We offer fast-track recertification training in Toronto to help you keep your skills current before they expire.
About the Author
Ashkon Pourheidary, B.Sc. (Hons) — Co-Founder, Coast2Coast First Aid & Aquatics
Ashkon has been a certified First Aid and CPR instructor since 2011 and an Instructor Trainer since 2013. He is also a certified Emergency Medical Responder (EMR) instructor, Psychological First Aid instructor, and BLS (Basic Life Support) instructor. Ashkon graduated with honours with a Bachelor of Science in Neuroscience from the University of Toronto in 2016. As co-founder of Coast2Coast First Aid & Aquatics, he has helped grow the organization to over 30 locations across Canada and into the United States. Ashkon has served on the First Aid Council for the Canadian Red Cross. He spends his time coaching the team of over 100 instructors at Coast2Coast to ensure that students training at Coast2Coast locations receive the best training experience. Connect on LinkedIn