Executive Summary: A stroke, often called a “brain attack,” is a profound medical emergency where applying the 120-second response rule can drastically alter a patient’s outcome. With approximately 1.9 million brain cells dying every minute a stroke goes untreated, recognizing symptoms via the BE FAST method and calling 911 immediately is paramount. Our American Red Cross and AHA-approved First Aid courses rigidly adhere to the CSA Z1210:24 standard, equipping you with Basic and Intermediate certifications—valid for two years—to confidently manage life-threatening neurological emergencies.
A stroke is a true medical emergency where time is critical. Each minute without treatment increases the risk of lasting brain damage, long-term disability, or even loss of life. Recognizing the warning signs quickly and getting emergency care right away greatly improves the chances of survival and recovery. Below, we’ll cover what triggers a stroke, the key symptoms to watch for, and the first aid actions you can take until medical professionals arrive.
To truly understand the gravity of this condition, it is vital to recognize that a stroke is essentially a brain attack. Just as a heart attack deprives the heart of vital resources, a stroke deprives the brain of oxygen-rich blood. According to organizations like the American Stroke Association and the National Heart, Lung, and Blood Institute, every minute that a stroke goes untreated, approximately 1.9 million brain cells die. This staggering statistic underscores why immediate treatment is not just a recommendation—it is an absolute necessity.
What Causes a Stroke?
A stroke happens when the essential blood supply to part of the brain is interrupted or severely reduced. The brain relies on a vast network of blood vessels, including the major carotid arteries in the neck, to deliver oxygen and nutrients. When this blood flow is impeded, brain tissue begins to suffer almost instantly. Without oxygen-rich blood, brain cells begin to die within minutes, leading to potentially irreversible brain damage or severe neurological disorders.
Understanding how strokes happen requires looking at the three primary categories. There are three main types of strokes that you should be aware of, each with distinct causes but equally devastating potential impacts:
Ischemic Stroke
Ischemic Stroke – This is by far the most common type, as ischemic strokes account for about 85% of all strokes. An ischemic stroke occurs when a blood vessel supplying blood to the brain is blocked or narrowed. This dangerous blockage is most often caused by a blood clot (thrombus) that forms directly in the brain arteries, or by fatty deposits (plaque) that build up in blood vessels and break off, traveling to the brain. When these vessels become obstructed, the localized brain tissue is starved of oxygen, initiating a rapid decline in cellular health.
Hemorrhagic Strokes
Hemorrhagic Stroke – A hemorrhagic stroke occurs when a weakened blood vessel in the brain leaks or bursts, causing bleeding directly in or around the brain. This escaped blood creates immense pressure on the surrounding brain cells, damaging them rapidly. Hemorrhagic strokes can result from conditions that heavily affect blood vessels, such as chronic high blood pressure, trauma, blood-thinning medications, or aneurysms (weak, bulging spots in the vessel walls). Though less common than ischemic events, they are notoriously deadly and require highly specialized emergency medical care.
Mini Stroke (Transient Ischemic Attack)
Transient Ischemic Attack (TIA) – Often called a “mini stroke,” a TIA is a temporary period of symptoms similar to those of a full stroke. A TIA is caused by a temporary decrease in blood supply to part of the brain, usually due to a fleeting blood clot. While the acute stroke symptoms may disappear and only last a few minutes to hours, a TIA is a blaring, critical warning sign of a future, much more severe stroke. Anyone experiencing TIA symptoms must receive an urgent medical evaluation, as ignoring it drastically increases the risk of a catastrophic brain attack in the near future.
Register for First Aid & CPR Training
Register Now
Stroke Signs and Symptoms
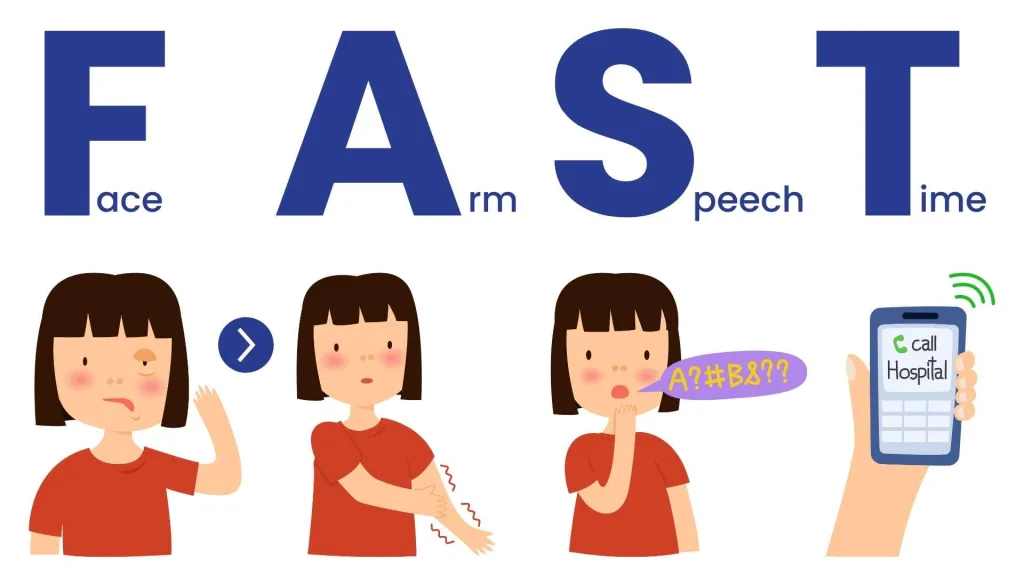
The effects of a stroke depend heavily on the specific part of the brain affected and how severe the oxygen deprivation is. Because immediate treatment is paramount, recognizing the warning signs is a fundamental skill. The F.A.S.T. acronym is an incredibly easy and effective way to remember the most common warning signs:
- F – Face: Sudden drooping or numbness on one side of the face. Face drooping is a common symptom of stroke that can be identified easily. To test this, ask the person to smile broadly and check for unevenness or a lopsided expression.
- A – Arms: Sudden numbness or arm weakness. Arm weakness can indicate a stroke when you ask the person to raise both arms and you observe if one arm drifts downward. If one arm is weak or cannot be raised at all, this is a major red flag.
- S – Speech: Speech difficulty, such as sudden trouble speaking and understanding what others are saying. Speech slurred or garbled words are a classic sign. Speech difficulty can be assessed by asking the person to repeat a simple sentence and checking for slurred speech or inability to articulate.
- T – Time: Time is critical—call 911 immediately if you see any of these signs. Do not wait to see if symptoms stop or disappear. Every second counts.
Signs of a Stroke: Expanding the Warning Signs
While the FAST acronym covers the most prevalent symptoms, medical professionals also encourage the use of the expanded BE FAST acronym to spot stroke symptoms, which includes Balance and Eyesight. First Aid training for stroke response should include the F.A.S.T. and BE FAST methods to help identify stroke symptoms quickly.
Common stroke signs beyond the face, arms, and speech include:
- Balance Loss: Sudden dizziness, sudden trouble walking, or a profound loss of balance and coordination can indicate a stroke. The victim may stumble or be completely unable to stand.
- Eyesight Changes: Problems seeing in one or both eyes can be a symptom of a stroke. Sudden blurred, double vision, or a complete loss of vision in one or both eyes may indicate a severe blockage in the brain’s visual processing centers.
- Sudden Numbness: Paralysis or numbness of the face, arm, or leg on one side of the body can indicate a stroke. This unilateral (one-sided) weakness is a hallmark of brain attacks.
- Sudden and Severe Headache: A severe, sudden headache with no known cause can be a symptom of a stroke. Often described by patients as the “worst headache of your life,” this sudden severe headache is particularly associated with hemorrhagic strokes.
- Sudden Confusion: A sudden loss of cognitive function, sudden confusion, or sudden memory loss may also indicate a stroke, especially if the victim cannot comprehend simple instructions.
Stroke Symptoms in Women and Children
It is important to understand that strokes do not always present identically in every demographic. While the classic signs remain the most common, women can present with unique stroke symptoms. These “nontraditional” signs in women may include sudden hiccups, nausea, sudden chest pain, or general body weakness during a stroke. Because these symptoms can mimic other illnesses like the flu or a heart attack, they are sometimes dangerously overlooked.
Similarly, pediatric strokes, though rare, do happen. Children may experience seizures, extreme sleepiness, or sudden vomiting along with standard stroke signs, according to current American Stroke Association guidelines.
Call 911: Emergency Medical Care is Vital
If you suspect someone is having a stroke, call 911 immediately. This cannot be overstated. A stroke is a medical emergency that can lead to permanent brain damage or death. Delaying treatment for a stroke can lead to increased risk of permanent disability.
Do not drive to the hospital. First Aid training should heavily emphasize the importance of not driving to the hospital if someone is suspected of having a stroke. When you call emergency services, medical personnel and first responders can begin treatment for a stroke even before reaching the hospital, which is crucial for patient outcomes. They can monitor vital signs, manage breathing, and communicate directly with the emergency room so the stroke team is ready the moment the ambulance arrives.
When you call 911, carefully note the time when stroke symptoms first appear. This information is absolutely critical for doctors to determine treatment options. The best stroke treatments, specifically powerful clot-busting medications, are most effective when administered within 3 hours of the first symptoms (and up to 4.5 hours for certain eligible patients).
⚠️ Compliance Alert for Employers
To remain fully compliant with the CSA Z1210:24 standard, ensure you register your staff for the correct first aid level: Basic (formerly Emergency) for standard workplaces, or Intermediate (formerly Standard) for larger facilities. Proper training ensures your team can recognize stroke warning signs and coordinate emergency medical attention swiftly.
First Aid for Stroke Emergencies
If you observe someone experiencing stroke symptoms, do not wait to see if the symptoms go away. Immediate medical attention is essential. Follow these first aid steps until emergency responders arrive:
- Call 911 right away. Calling 911 immediately can initiate life-saving treatment even before reaching the hospital.
- Note the time symptoms began. Note the time symptoms first started, as treatments are most effective within 4.5 hours.
- Keep the person comfortable. Loosen any restrictive clothing on a suspected stroke victim to assist with breathing. If they’re awake, help them sit or lie down in a safe, supported position.
- Do not give them food or drink. Avoid administering medications, food, or drink to a stroke patient, as this may cause swallowing problems. The paralysis can affect their throat, leading to a severe choking hazard.
- Stay calm and monitor their condition. Offer reassurance. Keep talking to them to monitor their cognitive state.
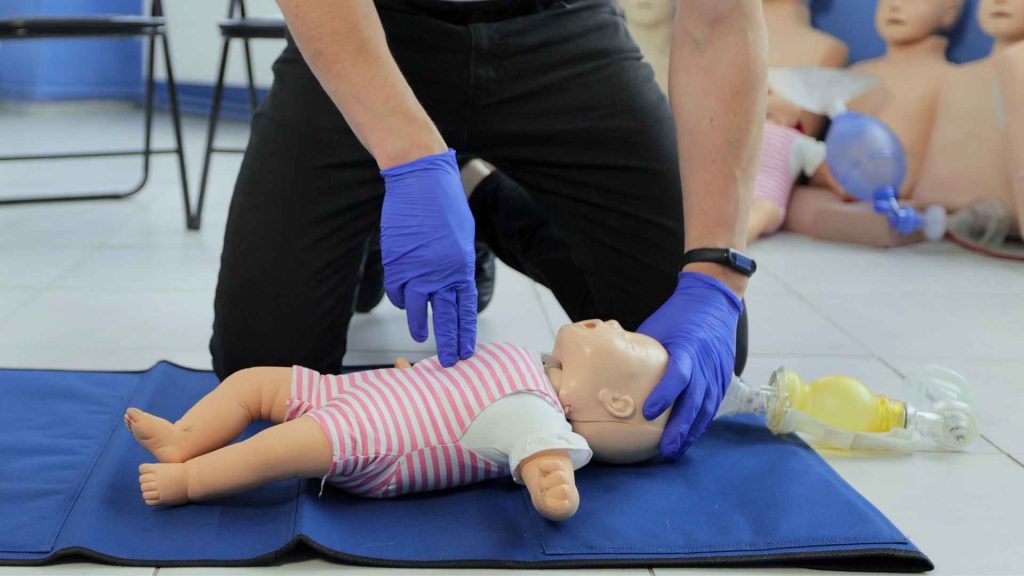
- Be prepared to give CPR. If the person loses consciousness and stops breathing normally, begin life saving treatment by performing high-quality CPR immediately and deploy an AED if one is available.
Remember: You cannot tell the type of stroke by looking at the person, so always treat every stroke as a life-threatening emergency where every minute counts.

Stroke Treatments and the Emergency Room
Upon arriving at the emergency room, doctors will rapidly assess the acute stroke. They will likely conduct a series of neurological exams and imaging tests, such as a CT scan or MRI, to determine if the stroke is ischemic or hemorrhagic. They may also perform blood tests to check clotting times and blood sugar levels, or a carotid ultrasound to look for plaque buildup in the carotid arteries.
If the stroke is ischemic and the patient arrives quickly, doctors may administer a clot-dissolving medicine called tPA (tissue plasminogen activator). Timely treatment of a stroke can significantly reduce brain damage and improve outcomes. For severe blockages, surgeons may perform an endovascular procedure to physically remove the blood clot. For hemorrhagic strokes, treatments focus on controlling bleeding and reducing pressure in the brain, sometimes requiring surgical intervention to repair the ruptured vessel.
| Course Level (2026 Standards) | Target Audience | Duration | Validity |
|---|---|---|---|
| Basic (Emergency) First Aid & CPR | General public, office workers, community volunteers | 1 Day | 2 Years |
| Intermediate (Standard) First Aid & CPR | Designated safety officers, industrial workers, teachers | 2 Days | 2 Years |
| Basic Life Support (BLS) | Healthcare providers, clinical staff, first responders | 4-5 Hours | 1 Year |
Stroke Risk Factors
Preventing a stroke begins with understanding your personal risk profile. Stroke risk factors are generally divided into two categories: those you cannot change and those you can manage.
Uncontrollable Risk Factors:
- Age: Age increases the risk of having a stroke. The likelihood roughly doubles every decade after age 55.
- Family History: A family history of strokes or heart attacks increases the likelihood of having a stroke.
- Gender: Men are at a higher risk of stroke than women. However, because women generally live longer, more women ultimately die from strokes each year.
- Race: African-Americans have a higher risk of stroke compared to other racial groups, largely due to higher rates of blood pressure and diabetes in these demographics.
Heart Disease and Manageable Stroke Risk
Many strokes are highly preventable through lifestyle changes and medical management.
- High Blood Pressure: High blood pressure is a significant risk factor for stroke. It is the leading cause of stroke, as it places constant, damaging stress on blood vessel walls.
- Heart Disease: Certain forms of heart disease increase the risk of stroke. Notably, a condition called atrial fibrillation (an irregular heartbeat) allows blood to pool and form clots in the heart, which can then travel to the brain.
- Smoking: Smoking increases the risk of stroke significantly by damaging blood vessels and making blood more prone to clotting.
- Diabetes: Poorly controlled diabetes increases the risk of stroke by causing destructive changes to blood vessels throughout the body.
- Weight and Diet: Being overweight increases the risk of stroke, often tying into high cholesterol and hypertension. Maintaining a healthy weight through diet and exercise is vital.
- Physical Inactivity: Physical inactivity increases the risk of stroke. Regular cardiovascular exercise keeps the circulatory system resilient.
- Lifestyle Choices: Heavy alcohol consumption is associated with a higher risk of stroke. Furthermore, obstructive sleep apnea is a risk factor for stroke, as the repeated drops in oxygen during sleep put heavy stress on the cardiovascular system.
Be Prepared: Learn First Aid & CPR
A stroke can happen anytime, anywhere. Training in stroke response is essential for workplaces and community groups to ensure safety. First Aid training should include stroke response as part of its curriculum. In fact, comprehensive CPR courses often incorporate stroke recognition and response training to ensure participants are well-rounded lifesavers.
Acting quickly in response to a stroke can significantly improve outcomes for the patient. Being trained in First Aid and CPR gives you the confidence to respond in an emergency—whether it’s recognizing the early signs of a stroke, understanding when to call 911, or taking action until EMS arrives.
At Coast2Coast, we provide American Red Cross First Aid and CPR certification courses designed to prepare you for real-life emergencies. By participating in First Aid training, participants learn to call 911 immediately if they suspect someone is having a stroke and understand that time is critical in treating a stroke to minimize brain damage.
Complete Your First Aid & CPR Course Today!
Recommended Courses
First Aid & CPR Courses
Coast2Coast CPR/AED Courses Information
Private First Aid & CPR/AED Programs
Frequently Asked Questions
Question 1: What are the most common signs of a stroke?
Answer: Common stroke signs include sudden numbness or weakness in the face, arm, or leg (especially on one side of the body), sudden confusion, trouble speaking, vision changes, sudden dizziness, or a severe headache.
Question 2: What does the F.A.S.T. acronym mean?
Answer: The acronym F.A.S.T. helps identify stroke symptoms rapidly: Face drooping, Arm weakness, Speech difficulty, and Time to call 911 immediately if any of these occur.
Question 3: How do you check for face drooping during a stroke?
Answer: Face drooping is a common symptom of stroke that can be identified by asking the person to smile. Check to see if one side of their face is uneven, numb, or hanging lower than the other.
Question 4: How can I test a person for arm weakness?
Answer: Arm weakness can be tested by asking the person to raise both arms. Observe if one arm drifts downward or if they are entirely unable to lift one arm due to sudden weakness or paralysis.
Question 5: What is an ischemic stroke?
Answer: An ischemic stroke occurs when a blood vessel supplying blood to the brain is blocked or narrowed, typically by a blood clot. Ischemic strokes account for about 85% of all strokes.
Question 6: How many brain cells die during a stroke?
Answer: A stroke is a devastating brain attack. Every minute that a stroke goes untreated, approximately 1.9 million brain cells die, highlighting why emergency medical attention is so urgently required.
Question 7: What is the treatment window for a stroke?
Answer: Stroke treatments, such as clot-busting medications, are most effective when administered within 3 hours (and up to 4.5 hours for certain patients) of the first symptoms appearing.
Question 8: Why shouldn’t I drive someone to the hospital if they are having a stroke?
Answer: You should call 911 immediately rather than driving. First responders can begin life-saving treatment for a stroke even before reaching the hospital and can alert the emergency room to prepare for immediate intervention.
Question 9: Do women experience different stroke symptoms than men?
Answer: Yes, women can present with “nontraditional” signs such as sudden hiccups, severe nausea, sudden chest pain, or sudden general body weakness, in addition to the standard FAST symptoms.
Question 10: Are there racial disparities in stroke risk?
Answer: Yes. Statistically, African-Americans have a higher risk of stroke compared to other racial groups. This is often linked to higher underlying rates of high blood pressure and diabetes within the demographic.
Question 11: What is a Transient Ischemic Attack (TIA)?
Answer: A transient ischemic attack (TIA) or “mini-stroke” is a temporary decrease in blood supply to part of the brain. Symptoms may disappear quickly, but it is a critical warning sign of a major future stroke.
Question 12: Can a headache be a sign of a stroke?
Answer: Yes. A sudden and severe headache with no known cause, often described as the worst headache of your life, can be a symptom of a stroke, particularly a hemorrhagic stroke where bleeding occurs in the brain.
Question 13: Should I give a stroke victim food or water?
Answer: No. Avoid administering medications, food, or drink to a stroke patient. Strokes frequently cause sudden paralysis of the throat muscles, leading to severe swallowing problems and choking hazards.
Question 14: What does the “BE” in BE FAST stand for?
Answer: The “BE” stands for Balance and Eyesight. Loss of balance or coordination, sudden trouble walking, or sudden blurred, double, or loss of vision in one or both eyes may indicate a stroke.
Question 15: Are strokes more common in men or women?
Answer: Men are at a higher risk of experiencing a stroke than women at younger ages. However, because women generally have a longer life expectancy, more women ultimately suffer and pass away from strokes overall.
Question 16: What is a hemorrhagic stroke?
Answer: A hemorrhagic stroke occurs when a weakened blood vessel in the brain leaks or bursts, causing bleeding in the brain. This is often the result of chronic high blood pressure or a ruptured aneurysm.
Question 17: How does First Aid training help with strokes?
Answer: First Aid training teaches the F.A.S.T. method to spot stroke symptoms quickly, emphasizes the importance of calling 911 immediately, and trains you to perform CPR if the victim loses consciousness and stops breathing.
Question 18: What are the main modifiable risk factors for a stroke?
Answer: Modifiable stroke risk factors include high blood pressure, smoking, being overweight, physical inactivity, heavy alcohol consumption, and poorly controlled diabetes or heart disease (like atrial fibrillation).
Question 19: Do children get strokes?
Answer: Yes, though rare, pediatric strokes do occur. Children may exhibit symptoms like seizures, extreme sleepiness, or sudden vomiting alongside traditional stroke signs like face drooping or arm weakness.
Question 20: How long is an American Red Cross First Aid certification valid?
Answer: Basic and Intermediate First Aid and CPR certifications obtained through authorized providers are valid for two years, ensuring responders stay updated on the latest emergency medical care protocols like the CSA Z1210:24 standard.
About the Author
Ashkon Pourheidary, B.Sc. (Hons) — Co-Founder, Coast2Coast First Aid & Aquatics
Ashkon has been a certified First Aid and CPR instructor since 2011 and an Instructor Trainer since 2013… Connect on LinkedIn